Atopic Skin Disease, Eczema Treatment Guidelines, and Lichenification
|
author/source: DrB
It is confusing that three terms are used to describe one skin condition: atopic skin disease, atopic eczema and atopic dermatitis. Strictly speaking the term atopic skin disease is equivalent to the terms atopic eczema and atopic dermatitis. Atopic skin disease aims to draw attention to the lichenification of the skin in persistent, or chronic, atopic eczema, also known as atopic dermatitis. There can be also confusion about the chronic nature of atopic eczema. The word chronic means longstanding, from the Latin and Ancient Greek words for time. In medicine chronic is contrasted with acute, which means recent and short-lived. Usually the confusion over chronic occurs if the word is used to mean severe. Both acute and chronic medical conditions can be described as severe, moderate or mild, depending on their seriousness. Longstanding or chronic conditions may over time come and go. They relapse, and remit. The relapses and remissions may be related to treatment, which may be required for the acute relapse phase only. However treatments are sometimes also recommended for a condition when it is in remission if it is shown that this can prevent acute relapses. Atopic eczema is described as a chronic condition, in treatment guidelines for example, because typically it recurrently relapses and remits over time. |
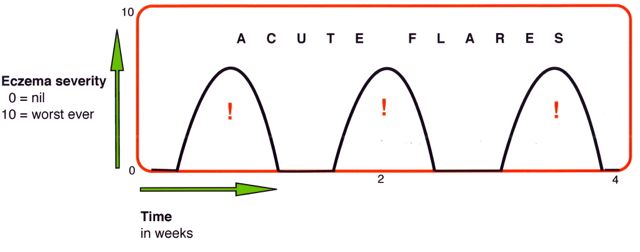 |
| Over a period of weeks several acute flares of inflammation can occur. Treatment guidelines especially focus on the effective treatment of acute eczema, with emollients and topical steroids for example. Usually little is said of the skin condition between acute episodes, except to say that the continuous appropriate use of emollients and soap substitutes to prevent the skin from drying can reduce the risk of acute relapses. Knowing about trigger factors and how to manage them is also important. But one of the striking characteristics of atopic eczema can be an associated thickening of the skin called lichenification. This is due to recurrent mechanical damage caused by scratching, and it can occur regardless of the effectiveness of the treatment of acute eczema. Lichenification occurs in other skin conditions where regular skin rubbing and scratching occurs. |
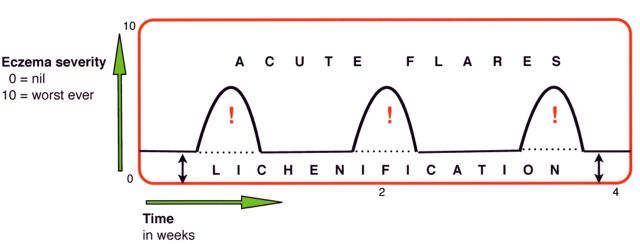 |
| The Combined Approach to atopic eczema combines optimal topical treament with habit reversal to tackle the habitual scratching behaviour that causes lichenification. Atopic eczema is chronic, or long-standing, in two different ways:
OR
When we recommend at routine assessment asking how much atopic eczema present on any given day is acute, and how much is chronic, we mean "chronic" in the second sense above. We ask
Without habit reversal the lichenification of chronic eczema remains untreated. As a major trigger factor for episodes of acute eczema, it is a significant cause of the negative quality of life effects of having atopic eczema. We recommend that guidelines for the treatment of atopic eczema should in future make reference to lichenification and its effective treatment. SEE ALSO:
|
